Chapter 26: Acute oncology
Skip chapter table of contents and go to main content
Neutropenic sepsis
Definition
Neutropenic sepsis is defined as a temperature greater than 38°C with a neutrophil count of less than 0.5 × 10⁹/L in a patient receiving systemic anticancer treatment (NICE [206]).
Related theory
Patients with neutropenia are vulnerable to invasive infection, which can be rapidly overwhelming, causing septic shock and death (Clarke et al. [37]). It is acknowledged that neutropenic sepsis, as with all forms of sepsis, is a medical emergency. Early recognition combined with urgent administration of intravenous antibiotics is essential to ensuring a good patient outcome (Ford and Marshall [81], NICE [206]).
Despite this, neutropenic sepsis remains a major and one of the most common complications of cancer chemotherapy, with an associated mortality rate ranging from 2% to 21% (Ford and Marshall 2014, National Institute for Clinical Excellence [NICE] and the National Collaborating Centre for Cancer [206]). The condition contributes to 50% of deaths associated with leukaemia, lymphomas and solid tumours (Viscoli [300]). Younger patients and patients on corticosteroids are more likely to present with ill‐defined symptoms and, despite baseline observations being abnormal, may look quite well (Mort et al. [189]). Bacterial infections are common in patients with febrile neutropenia, but fungal sources are increasingly prevalent (Ford and Marshall [81]). There is considerable variation in symptoms, which can include a temperature of 101°F (38.3°C) or more and an absolute neutrophil count (ANC) less than 500 per mm3 (0.5 × 109/L) (Ford and Marshall [81], Quint [239]). The defining presenting features of general sepsis are two or more of the following symptoms: fever (> 38°C) or hypothermia (< 36°C), tachypnoea (> 21–24 breaths per minute), tachycardia (91–130 beats per minute [bpm]), hypotension (systolic BP < 90 mmHg or 40 below normal) or oliguria for 12–14 hours (NICE [209]). However, in many patients with neutropenia, particularly those taking corticosteroids, the systemic inflammatory response to infection is attenuated, meaning that the diagnostic criteria for sepsis might not be fulfilled and a clear focus of infection might not be found. For this reason, there must be a high index of suspicion for infection in all patients undergoing chemotherapy who become unwell, even in the absence of fever. The only evidence of neutropenic sepsis might be a general deterioration in condition, or non‐specific signs such as confusion. The neutrophil count typically reaches its nadir approximately 5–7 days after administration of SACT, at which time patients are particularly susceptible to infection. Once sepsis is established a situation develops in which oxygen consumption at tissue level rises and cannot be met by the circulation, which will eventually show as tachycardia, hypotension, hypoxia and tachypnoea (Dellinger et al. [57]).
Investigations
Although it is important to undertake a thorough investigation into the presenting complaint with this oncological emergency, time is of the essence (NICE [206], [209]). The national recommendation for the initial management of sepsis (± neutropenia) is to give initial empiric therapy within 1 hour of presentation of the patient to a healthcare professional (Dellinger et al. [57], NICE [206], [209]). Although blood cultures should be taken initially it must be appreciated that it will take 24–48 hours to get a result and treatment should start immediately. Specification of antibiotics can be done once results are available.
A high index of suspicion of neutropenic sepsis must be acted upon if a cancer patient presents feeling unwell, with or without a temperature, on active cancer treatment, or if they have received treatment in the last 6 weeks (Clinical Knowledge Summaries [CKS] [41]). A simple history of the presenting complaint will provide information regarding the speed of onset of symptoms along with any co‐morbidities (Marrs [165]). Baseline observations (including EWS) plus initial blood work on presentation should include (Dellinger et al. [57], NICE [206], [209]):
- Temperature – although fever is usually the alerting sign (37.5°C on more than two occasions or 38°C on one occasion), patients may also present with hypothermia or confusion.
- Pulse – manual as well as via a monitor as this will inform of the regularity, strength and contour.
- Oxygen saturations – confirmed on blood gas.
- Respiratory rate – this is the simplest observation to take and the one that will change most quickly in a deteriorating patient.
- Blood pressure – looking for signs of septic shock. It may be that the patient is hypertensive prior to becoming hypotensive.
- Conscious level – AVPU.
- IV access and blood tests:
- Lactate (venous blood gas is appropriate at this point), FBC, coagulation screen, U&Es, LFTs (including albumin), glucose (also take a capillary blood glucose level), calcium, magnesium, CRP.
- Full septic screen:
- Blood cultures – from peripheral vein and central venous access device (if in situ).
- Urine dip and specimen.
- Swab all skin breaks.
- Stool if the patient has complained of loose motion in last 24 hours.
- Commence fluid balance monitoring.
Certain drugs may mask these signs, such as beta blockers which will reduce tachycardia allowing hypotension to develop more easily. Corticosteroids and NSAIDs (e.g. regular ibuprofen) may affect temperature regulation leading to a minimal rise in temperature that would otherwise be easy to ignore (de Naurois et al. [55]). If respiratory symptoms are present, chest radiography is recommended, although it may not detect an infiltrate until the patient's ANC has improved enough to enable an inflammatory response (Hughes et al. [115]). This, however, can wait until empiric antibiotics are given along with antipyrexials (if required).
Management
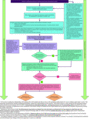
Suspected neutropenic sepsis should be treated as a medical emergency and empiric antibiotic therapy commenced immediately, prior to blood results (NICE [206]). Local policy will guide the initial empirical management of sepsis which will normally include monotherapy using a broad‐spectrum agent such as piperacillin with tazobactam (NICE [206]). See Figure 26.7 for an example of a neutropenic sepsis management pathway.
The role of the cancer nurse in this group of patients is to respond immediately when neutropenic sepsis is suspected and ensure that it is acknowledged as a medical emergency. Early recognition and treatment of sepsis is key to improving outcomes. In order to support the effective and efficient management of patients in suspected severe sepsis, six basic therapies (bundles) were developed based on best practice guidelines (NHS England [201]). The use of ‘bundles’ has been shown to simplify the complex processes of the care of patients with severe sepsis (NHS England [201]). A bundle is a selected set of elements of care that, when implemented as a group, have an effect on outcomes beyond implementing the individual elements alone (Surviving Sepsis [279]). One such bundle dealing with basic therapies, the ‘sepsis six’ (Table 26.12), has been shown to improve outcomes in septic patients. If the six factors are completed within the first hour following recognition of sepsis, the associated mortality has been reported to reduce by as much as 50% (Surviving Sepsis [279]).
Table 26.12 Severe sepsis care bundle
| Procedure | Rationale |
|---|---|
| Oxygen: start with high flow (15 L via non‐rebreathe mask and titrate down) – target saturations > 94% | Intended to restore the imbalance between oxygen supply and demand to the tissues |
|
Fluid resuscitation: give boluses of 0.9% sodium chloride (500 mL) over 15 minutes
Observe response and repeat as necessary until hypotension/organ dysfunction is improved (up to max 1.5–2 L then call senior doctor/ICU) | Intended to restore the imbalance between oxygen supply and demand to the tissues |
Blood cultures: take at least two sets, including at least one from a fresh venepuncture
| Assists with identification of sepsis source, systemic and CVAD related (NICE and the National Collaborating Centre for Cancer [206], Surviving Sepsis [279]) |
| IV antibiotics as per trust/local guidelines: ensure they are given immediately (within 1 hour of suspected neutropenic sepsis) | Decreases the risk of mortality and morbidity (NICE [206]) |
Arterial blood gas to measure lactate: a venous sample is OK if respiratory status is stable
| A failure of lactate to improve with therapy is indicative of a poor outcome. Lactate clearance has been shown to correlate positively with survival |
Take bloods for FBC, U&Es, clotting
| Enables assessment of patient condition and management (NHS England [201], NICE [206]) |
Commence hourly fluid balance
|
Risk of AKI due to sepsis (Reilly et al. [246])
Increased risk of bleeding if platelet count < 50 × 10⁹/L |
| Source: Adapted from NHS England (2013). |
Neutropenia has been found to be independently associated with a higher risk of AKI (urine output of less than 0.5 mg/kg/h for 6 hours) therefore close monitoring of the patient's haemodynamic status, including urine output, is essential (Reilly et al. [246]). Combined with the risk of hypotension in sepsis, fluid resuscitation may be required. If the patient's history includes oliguria or they present with hypotension, fluid resuscitation may be required. Treating hypotension through fluid resuscitation should be a central tenet in treating sepsis (Daniels [52]). Fluid resuscitation is as follows:
- Give 500 mL of 0.9% sodium chloride (NaCl) over 15 minutes. There is no evidence to suggest the use of a colloid is any more effective.
- Observe the patient and check vital signs at end of infusion and then every 15 minutes.
- If a satisfactory response has been achieved, give maintenance fluids to cover general anticipated fluid losses.
- Continue monitoring every 15 minutes for the first hour, then every 30 minutes for the second hour, and then hourly.
- If there is no response and jugular venous pressure (JVP) is not raised, repeat the fluid challenge.
- If a third fluid challenge is required, the clinical team and critical care outreach team should have been called.
NICE and the National Collaborating Centre for Cancer ([206]) recommend that immediately following empiric IV antibiotic treatment the patient be risk assessed using a validated tool such as the Multinational Association for Supportive Care in Cancer (MASCC) scoring system for grading neutropenic sepsis. Table 26.13 shows how this has been adapted for use at The Royal Marsden to determine the risk of prolonged septic complications to guide ongoing management. If a patient is risk stratified as having low‐grade neutropenia (a score of > 21) outpatient management with oral antibiotics and robust follow‐up with access to expert cancer triage in the ambulatory setting may be appropriate (Cooksley et al. [45], NICE and the National Collaborating Centre for Cancer [206]). There is currently no consensus as to the period of monitoring low‐risk patients should undergo prior to being discharged from hospital; this ranges from 24 to 48 hours (Freifeld et al. [86]). In high‐risk patients (a score of < 21) or where an organism has been isolated, treatment should be continued for 5 days (NICE [206]).
Table 26.13 The metastatic spinal cord compression (MASCC) scoring system adapted for local use at The Royal Marsden for grading neutropenic sepsis risk
| Yes | No | Scorec26-note-0009 | ||
|---|---|---|---|---|
| Does the patient have a solid tumour or lymphoma (except Burkitt lymphoma)? | 4 | 0 | ||
| Is the patient dehydrated or requiring IV fluids? | 0 | 3 | ||
| Is the systolic BP < 90 mmHg? | 0 | 5 | ||
| How sick is the patient? | No/mild symptoms | 5 | 0 | |
| Moderate symptoms | 3 | 0 | ||
| Severe symptoms | 0 | 0 | ||
| Is the patient aged < 60 years? | 2 | 0 | ||
| Does the patient have chronic obstructive pulmonary disease? | 0 | 4 | ||
| Did the patient develop febrile neutropenia while an inpatient? | 0 | 3 | ||
| Total MASCC score |
| * | Points attributable to burden of illness are not cumulative. The maximal theoretical score is therefore 26. A threshold of ≥ 21 points defines ‘low risk’. Source: NICE ([206]). |
In addition, effective written local policies are essential to ensure a rapid response whenever neutropenic sepsis is suspected. Some patients may present with neutropenic sepsis via the Emergency Department, and in this situation clear protocols must be in place to manage these patients appropriately.
Patient education
Successful management of neutropenic sepsis requires prompt recognition of, and reaction to, potential infection. Patient education to promptly recognize symptoms is vital, with clear written instructions on when and how to contact the appropriate service (de Naurois et al. [55], Marrs [165], Mort et al. [189]). Also essential is educating outpatient and emergency departments to suspect sepsis until proven otherwise in any patient who presents with ill‐defined symptoms such as confusion or gastrointestinal upset and who has had SACT within 6 weeks of presentation (Ford and Marshall [81], Mattison et al. [170]).